In today’s healthcare landscape, academic medical centers (AMCs) and academic hospitals play a critical role in advancing research, education, and patient care.
Those familiar with AMCs understand the opportunities these unique healthcare models offer to the community. However, educating potential donors on the importance of AMCs and addressing the other challenges facing today’s academic healthcare organizations can be a complex task.
In this guide, we review everything you need to know to effectively engage donors in fundraising, communications, strategic planning, and relationship building to support the mission of academic medical centers:
- What is an Academic Medical Center?
- How to Unite Philanthropy and Academic Medical Centers
- 10 Compelling Benefits of Fundraising for Academic Hospitals
- Addressing the Challenges of Academic Hospitals
- Fundraising Tips for Academic Medical Centers
- Work with BWF to Enhance Your AMC Fundraising Strategy
What is an Academic Medical Center?
An academic medical center or hospital is a facility associated with a medical school or university that provides clinical care, education, and research opportunities for medical students, residents, and fellows. AMCs typically focus on advancing medical knowledge through research, clinical trials, and other innovative practices. They often offer specialized, high-quality care and are at the forefront of medical research and technology.
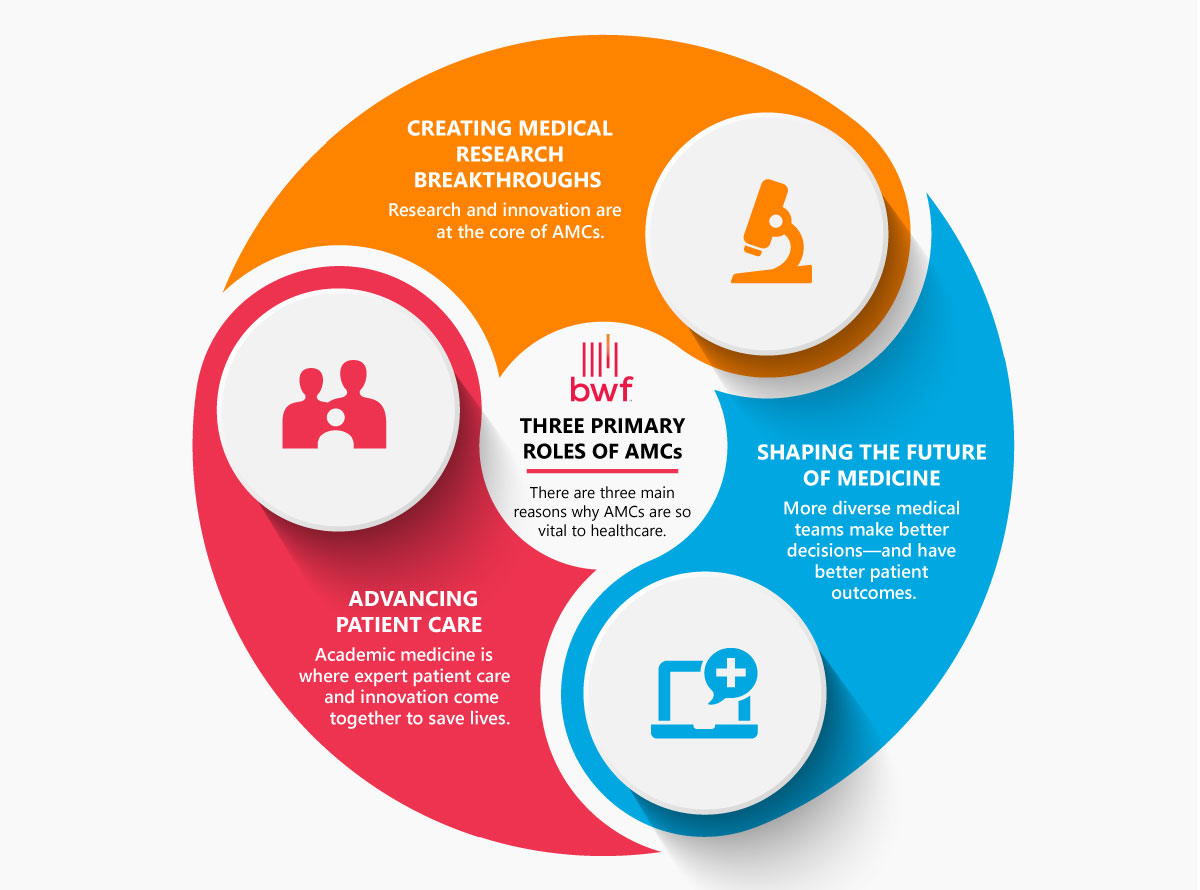
Three Primary Roles of Academic Medical Centers
AMCs provide many benefits to patients, the community, and the global healthcare landscape. Three main reasons make them vital to healthcare:
1. Creating Medical Research Breakthroughs
Research and innovation are at the core of AMCs. From NICUs to cancer research, which has saved more than 2.5 million people in the past 30 years alone, it all starts in academic medicine.
2. Shaping the Future of Medicine
More diverse medical teams make better decisions and have better patient outcomes. AMCs work to ensure tomorrow’s doctors have the innovative training they need to improve health everywhere.
3. Advancing Patient Care
Academic medicine is where expert patient care and innovation come together to save lives. In fact, patients treated at teaching hospitals have a higher survival rate compared to those treated at non-teaching hospitals.
Ultimately, one of your most essential roles as a fundraiser for an AMC is to never assume that your donors—or even your colleagues—fully understand what it means to be an AMC. Continually reinforcing the power and impact that AMCs have on our healthcare landscape and the unique nature of an AMC model is critical throughout your tenure as a development professional. Be loud, be proud, and always keep AMC points of pride at the forefront of your messaging.
How To Unite Philanthropy and Academic Medical Centers
AMCs provide many benefits, including best-in-class patient care, cutting-edge research, and top-tier education. But the magic really happens when philanthropy is added to the formula! Philanthropy can elevate the profile and impact of AMCs, providing funding for breakthroughs that wouldn’t be possible without the expertise of the AMC and donors’ passion.
As a fundraiser, you can align the goals of both leadership and philanthropists by highlighting the four major ways that monetary gifts support healthcare:

Funding Research
Philanthropy provides critical funding for research at AMCs, which can help accelerate medical breakthroughs, improve patient outcomes, and address healthcare challenges. Funding can support projects ranging from basic science research to clinical trials and translational research.
Donors can play a crucial role by providing seed funding for early-stage discovery work that often lacks support from government grants. This funding enables researchers to develop experimental ideas into potentially lifesaving solutions. And when donors contribute, their gifts can be leveraged to secure larger grant funding. This approach can be very inspiring, so we recommend using it as a key talking point when discussing support for research.
Enhancing Patient Care
Donor support of new programs, technologies, and facilities can enhance patient care at AMCs. Donations fund important developments such as purchasing new equipment, constructing new buildings or wings, and hiring additional staff.
Addressing Health Disparities
Philanthropy can help address health disparities by bolstering programs and initiatives that focus on underserved populations. These can include outreach and education programs, community-based research, and initiatives designed to increase access to healthcare services for vulnerable populations.
Providing Scholarships and Fellowships
Philanthropy can also support the education and training of the next generation of healthcare professionals by funding scholarships and fellowships. This can help attract and retain top talent, ensuring that patients receive the highest-quality care from well-trained and knowledgeable providers.
10 Compelling Benefits of Fundraising for Academic Hospitals
AMCs provide unique advantages and opportunities that you can leverage as a fundraising professional to inspire support. Providing donors with a thorough understanding of these benefits and how philanthropy supports healthcare is crucial to advancing the mission of your AMC.
1. Better Patient Outcomes
A study published in JAMA, “Association Between Teaching Status and Mortality in US Hospitals,” found that patients treated at “major teaching hospitals had lower adjusted mortality relative to nonteaching hospitals at 7, 30, and 90 days for all hospitalizations.”
The study presented several theories to explain this phenomenon, including the greater experience of teaching hospitals in treating specific conditions and their tendency to adopt new technologies at a faster rate than non-teaching hospitals.
2. Cutting-Edge Research
Research covers a vast array of areas and is typically thought of as a “bench to bedside and back again” approach at many AMCs. AMC research can be considered a three-legged stool consisting of basic research, translational research, and clinical trials.
3. Basic Research
Basic science is anything but basic. It is the root of all healthcare breakthroughs. Basic science includes disciplines such as biochemistry, microbiology, physiology, and pharmacology. At its core, basic science involves laboratory studies with cell cultures, animal studies, or physiological experiments. This type of research focuses on how the body functions in both health and illness, and is rooted in building hypotheses that can be tested and revised.
4. Translational Research
Translational research takes basic science to the next level. Once the fundamental principles of biological processes are understood, these discoveries can be applied to or directly translated into patient care.
Translational research includes:
- Preclinical Research: Preclinical research connects the basic science of disease with human medicine. During this stage, scientists develop model interventions to further understand the basis of a disease or disorder and find ways to treat it. Testing is carried out using cell or animal models of disease; samples of human or animal tissues; or computer-assisted simulations of drug, device, or diagnostic interactions within living systems.
- Clinical Research: Clinical research includes studies to better understand a disease in humans and relate this knowledge to findings in cell or animal models, testing and refinement of new technologies in people, testing of interventions for safety and effectiveness in those with or without disease, behavioral and observational studies, and outcomes and health services research. The goal of many clinical trials is to obtain data to support regulatory approval for an intervention.
- Clinical Implementation: The clinical implementation stage of translational science involves implementing interventions that have been demonstrated to be useful in a research environment into routine clinical care for the general population. This stage also involves implementation research to evaluate the results of clinical trials and identify new clinical questions and care gaps.
- Public Health: In this stage of translation, researchers study health outcomes at the population level to determine the effects of diseases and the impact of efforts to prevent, diagnose, and treat them. Findings help guide scientists in assessing the effects of current interventions and in developing new ones.
5. Clinical Trials
Clinical trials are one of the most well-known benefits of seeking care at an AMC and one of the reasons that many donors support AMCs. These trials:
- Allow patients to play an active role in their own healthcare.
- Grant patients access to new research treatments before they are widely available.
- Expand treatment options when standard therapy has been unsuccessful.
- Provide patients with expert medical care at leading healthcare facilities during the trial.
- Help others by contributing to the advancement of medical knowledge.
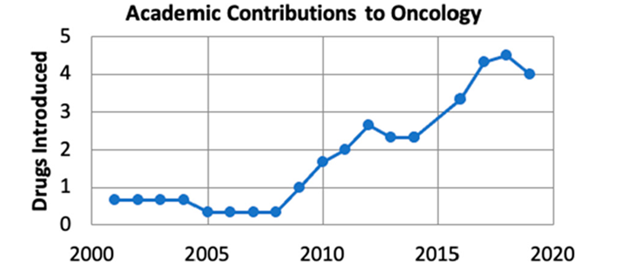
6. Drug Discovery
Thanks to the three-legged stool of basic science, translational science, and clinical trials, AMCs are also able to discover or repurpose drugs that lead to new treatment options. According to a study called “Rising Academic Contributions to Drug Development: Evidence of Vigor or Trauma?,” academic inventors or founders contributed to over a quarter of all medicines approved from 2001 through 2019.
7. Teaching the Next Generation
Teaching is one of the core tenets of an AMC. It is important to recognize that America is facing a healthcare worker shortage in the next decade, and AMCs are at the forefront of providing solutions.
According to the Association of American Medical Colleges (AAMC), America will face a shortage of up to 122,000 physicians by 2032. One-third of doctors today are over the age of 65 and nearing retirement. The nation’s 160 accredited medical schools and more than 400 major teaching hospitals and health systems are actively working to combat this issue.
To help address the looming doctor shortage, the nation’s medical schools have increased class sizes, and dozens of new medical schools have opened in the past decade. Altogether, these institutions have expanded enrollment by 31 percent to help ease the effects of the doctor shortage.
Medical schools and teaching hospitals are focused on educating more doctors, while also enhancing and refining their curricula and training. This ensures future healthcare professionals receive the necessary education to improve public health outcomes.
Examples include educating future doctors to address social determinants of health, responding to healthcare crises like the opioid epidemic, and providing care for ongoing healthcare needs such as obesity, smoking, diabetes, and heart disease.
8. Improving the Health and Well-Being of the Community
AMCs help the community in a myriad of ways, some of which are more obvious than others. According to a Supreme Court amicus brief, AMCs operate 71 percent of accredited level-one trauma centers and 98 percent of the nation’s 41 comprehensive cancer centers.
Teaching hospitals—which comprise only 5 percent of all hospitals in the United States—account for 69 percent of all burn unit beds, 63 percent of pediatric intensive care unit beds, 19 percent of all alcohol treatment unit beds, and 24 percent of all inpatient psychiatric beds.
AMCs also provide treatment for a disproportionately high percentage of Medicare and Medicaid beneficiaries, as well as those who are uninsured.
9. Addressing Health Disparities
AMCs play a significant role in addressing health disparities through research, education, and community engagement. Many of the nation’s medical schools and teaching hospitals also run innovative programs to address underlying social and economic factors in their communities that can lead to poor health. This includes providing access to healthy food, adequate housing, education, and transportation—all of which are social determinants of health.
Here are a few more examples of how AMCs address health disparities:
- Research: AMCs conduct research to understand the root causes of health disparities and develop interventions to address them. For instance, the University of California San Francisco established the Action Research Center for Health to research health disparities affecting vulnerable populations, such as low-income individuals and communities of color.
- Education: AMCs train the next generation of healthcare providers to address health disparities. For example, the University of Michigan Medical School has a curriculum that includes training on health equity and social determinants of health.
- Health Policy: AMCs can influence health policy to address health disparities. For example, the George Washington (GW) School of Medicine & Health Sciences offers a program called Public Health, Advocacy, and the Humanism in Medicine to train future healthcare professionals to effectively advocate for health equity.
10. Economic Benefits
AMCs contribute substantially to the economic health of their communities. One AAMC study showed that medical schools and teaching hospitals contributed $728 billion in gross domestic product (GDP)—about 3.23% of the national GDP
AMCs are often among the largest, if not the largest, employers in an area and typically employ a highly skilled workforce. They also indirectly create jobs through vendors and suppliers, and many offer workforce development programs and career ladder options that would otherwise be unavailable.
Addressing the Challenges of Academic Hospitals
In addition to the numerous benefits and opportunities that AMCs offer, there are real challenges and misconceptions to address when discussing AMCs with donors and community members.
Misconceptions and Fears
Given their unique nature, AMCs often have a mysterious air about them. What makes them so different from a local hospital? As you’ve read, there are many things! However, given that these misconceptions may lead patients to choose other hospitals or donors to give to organizations addressing many of the same problems as AMCs, it is vital that these notions be debunked quickly and directly.
Here are just a few examples of statements you may have heard or could hear in the future:
“I don’t want to be a guinea pig!”
Consider responding with, “Without clinical trials, today’s patients would be getting yesterday’s treatments, and there are so many great therapies afforded to us now. I understand your concern, although I am not a medical professional. Please consult with your physician and discuss your concerns about participating in a clinical trial. They will review all treatment options with you and can explain if and why a clinical trial may be a good option for you.”
“A student doctor? No, thank you!”
Consider responding with, “As an academic medical center, we are extremely fortunate to be training tomorrow’s physicians. The extensive training that they receive prepares them to deliver the very best patient care. There are also highly experienced faculty members who work closely alongside residents. Please discuss your fears with a physician, and I am sure you will be comforted by knowing how much oversight our experienced professionals will have as a part of your care team.”
“I’m not that sick. I don’t need a hospital like that.”
Consider responding with, “We hear that often, but statistics show that patients have better outcomes at academic medical centers—even those who are not critically ill. We encourage you to consult with one of our physicians to discuss your specific healthcare plan, and in partnership, you can determine if our hospital may be right for you.”
“I like my community hospital, and it seems to be cheaper.”
Consider responding with, “We encourage you to consult with one of our physicians to determine if the course of treatment at our hospital may be right for you or if the standard course of care can be delivered at your community hospital. Your care team, including our financial support staff, will help you better understand your options and what is best for your health, your convenience, and your financial situation.”
As a development officer, you should never overstep your boundaries or areas of expertise—especially when discussing medical decisions. However, since you may be confronted with these misconceptions while working alongside grateful patients, families, and concerned community members, it is important that you are prepared with answers.
Listen to the patient’s or donor’s concerns and collaborate with your medical leadership and faculty to understand how they can address these misconceptions.
Cost and Reimbursement
The cost of healthcare and reimbursement rates are very real issues that affect both patients and AMCs.
AMCs have above-average care costs due to the disproportionate share of uncompensated services they deliver and their staffing requirements. One study found that “hospitals with a substantial commitment to graduate medical education, major teaching hospitals, are about 10% to 20% more costly than nonteaching hospitals.” Additionally, payers may “nudge” patients to seek lower-cost facilities, and some insurance companies even exclude AMC facilities from narrow networks because of their higher costs.
It is essential to acknowledge that many of the benefits of an AMC also raise financial concerns for hospital leadership and management. AMCs receive lower Medicare and Medicaid reimbursements, and government funding for research has decreased significantly over the past few years. In today’s technology-savvy markets, the increased use of telemedicine has led to a decrease in in-person consultations, which in turn has resulted in a decline in revenue. Private systems are capturing a larger share of the market.
AMCs rely on government grants, philanthropy, and patient revenue; however, funding sources are uncertain and subject to change. While these are very real challenges, it can be persuasive to address them directly with donors to help inspire philanthropy.
Fundraising Tips for Academic Medical Centers
With a thorough understanding of the benefits and challenges facing AMCs, it is important to understand the ways in which you can impact philanthropy and leverage your messaging to increase support.
1. Communicate Clearly with Internal Stakeholders
Develop a clear message about your role as an AMC and share it broadly, as well as in strategic one-on-one efforts. Start by communicating within your organization and consider the following core groups for both input and approval:
- Your development teams
- Marketing and communications
- Your leaders
- Key clinicians and researchers
Develop a narrative about the innovations happening at your institution—what makes your AMC distinctive and invaluable to your patients and community. Ideally, your marketing and communications team can be key partners in this process. They may already have developed these materials.
Often, we use leadership, clinicians, and researchers to help us tell our compelling story to donors. Educate them on how they can share their professional passion with donors and connect it to the broader goals of an AMC.
2. Understand Your Donors on a Deeper Level
AMCs have the advantage of serving their communities through patient care and contributing to the world through research and education. Due to this breadth, AMCs can connect with a diverse range of donor populations.
Four of them include:
- Patients and Families: Those who have experienced the care of the AMC firsthand often want to give back.
- Former Students: Many residents, fellows, and other learners build strong bonds with each other, their departments, and the institution. Those connections can last a lifetime and are worth cultivating.
- Research-Focused Funders: Individuals and foundations who care about research may want to support the research happening at your institution, even if they aren’t in your backyard.
- Community Members: AMCs may find that even community members without a strong healthcare tie to the institution may want to support it. They are grateful to have an anchor institution like an AMC in their community and want to ensure it stays strong.
Create communication segments for each of these donor groups to send personalized messages. For example, you could focus your fundraising messages to former students on the idea that they can help newer learners achieve success, just as they have. Or, you can help grateful patients and their families understand how they can express their gratitude to the healthcare professionals who supported them throughout their medical journeys.
3. Create a Strategy for Broad Communication Efforts
Reinforce and reiterate the key messaging points about an AMC to the general public and donors alike. Consider incorporating the AMC message throughout your website, publications, and direct marketing materials to enhance your brand’s consistency and credibility.
Here’s an example from an annual giving appeal sent via direct mail:
“You can help us advance research, power innovation, support students in medical training, provide patient services for children and families, ease the journey of cancer patients, help us care for vulnerable populations across our region, and so much more.”
Additionally, videos are an impactful and visually appealing way to educate donors on what an AMC is and why your hospital is worthy of support. Consider interviewing patients, students, and healthcare professionals to add an emotional angle to your appeals.
4. Give Donors a First-Hand Look at Your Operations
Educating your donors about the power of AMCs can be a powerful cultivation tool. They can directly see how their support helps you achieve your mission of providing top-quality care to your community and high-value education to your students.
Demonstrate the power of research, education, and patient care through:
- Offering hands-on tours of research labs.
- Hearing from students.
- Talking to nurses about how they innovate to improve patient care.
- Attending a lecture or grand rounds.
- Meeting with a clinician who can talk about caring for patients, training residents, and researching an illness.
Optimizing the donor experience will help you foster long-term relationships with supporters, driving support for your healthcare mission for years to come.
Work with BWF to Enhance Your AMC Fundraising Strategy
BWF’s fundraising experts are trusted partners to children’s hospitals, academic medical centers, health systems, and other healthcare organizations. We understand the unique philanthropic challenges and opportunities of academic medical centers, as many of our consultants are former heads of development themselves.
We work with healthcare development teams to support initiatives like:
- Grateful patient programs
- Fundraising campaigns
- Major gift strategies
- CRM implementations
- Facilitated access programs
- Data science
- Prospect research
If you’re ready to develop an effective, long-term fundraising strategy for your academic hospital, contact our team to discuss your goals.
The Power of Academic Medical Centers and Solicitations
Ultimately, donors want to influence healthcare today and for the next generation. AMCs do just that, and how you position your solicitations can go a long way in inspiring donors. Showcase your AMC’s impact on your community, state, nation, and the world. Be bold with your solicitation, as your AMC’s mission is certainly bold and worthy of support.
By combining the benefits and opportunities outlined here with your hospital’s unique strengths, you are well-positioned to inspire philanthropy and shape the future of healthcare.
BWF can assist your AMC with insights and tools on how to overcome these challenges when cultivating philanthropic donors, helping you harness the power and innovation of an academic medical center. Please reach out to Kara Wagner, associate vice president, or Elizabeth Dollhopf-Brown, consulting partner. It’s a privilege to help.
Let’s Talk
Find out how BWF can partner with you to launch an effective healthcare fundraising strategy.